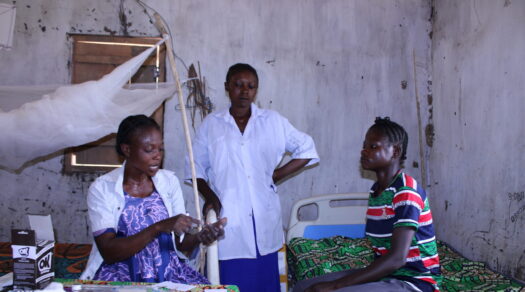The Bridge Between Belém and the Clinic
The Global Goal on Adaptation (GGA) now has a measuring stick. A decade after the Paris Agreement enshrined the GGA, countries finally agreed on a concrete measurement framework for tracking climate resilience at COP30 in Belém. After years of work, countries adopted adaptation indicators, including 10 focused on health.
- Change in the rate of mortality associated with heat exposure
- Change in the incidence of climate-sensitive infectious diseases
- Change in the annual rate of reported heat-related occupational injuries and deaths
- Extent of implementation of Mental Health and Psychosocial Support preparedness and response for climate change-sensitive events
- Number of destroyed or damaged health facilities and number of disruptions to health services associated with climate-related events
- Percentage of health facilities built or retrofitted to be climate resilient based on national, regional, or global guidance
- Universal Health Coverage: Coverage of essential health services
- Level of operationalization of climate-informed health early warning systems for climate change-related health risks accessible to vulnerable groups
- Level of implementation of climate change, health vulnerability, and adaptation assessment
- Proportion of the ministry in charge of health workforce that has received training on climate change and health in the last two years
These indicators give us a common language for monitoring everything from climate-sensitive infectious diseases to health facility resilience and, in a long-overdue move, the extent of mental health and psychosocial support for vulnerable populations.
But indicators alone don’t save lives. What matters is how governments translate these global metrics into national strategies, budgets, and services that reach communities on the frontlines.
The bridge between Belém and the clinic is built not with policy documents, but with political will, technical capacity, and sustained partnership. The key question is simple: will these indicators change what happens in hospitals, clinics, and communities when the next climate shock hits?


The COP30 Yardstick: A Political & Practical Win
Adopting these indicators represents a genuine breakthrough. For the first time, we have a universally agreed-upon standard to measure whether the world is adapting to climate change. The health indicators are particularly robust, calling for data on service continuity, health facility resilience, workforce capacity, and disease trends. However, as The Lancet rightly noted, this scientific success now faces the test of political will.
The adoption process was marked by last-minute maneuvering, with countries like Uruguay raising legitimate concerns about methodology and sovereignty. The critical question is whether the indicators can translate into real-world protection. The framework will live or die based on its ability to inform national plans, attract investment, and ultimately change outcomes for communities most exposed to climate risks. In other words, the framework must move from being a reporting exercise to becoming a decision-making tool.
From Global Metrics to Country Reality
This is where the global framework meets countries’ realities. The GGA indicators were never meant to be a prescriptive, one-size-fits-all reporting burden, but rather to “complement rather than replace existing monitoring systems.” The question is how to make that complementarity real.
The GGA’s call for tracking the “percentage of health facilities that are resilient” and the “coverage of essential health services supported by adaptation measures” is precisely the kind of system-strengthening Pathfinder excels at. For decades, Pathfinder International has worked alongside governments to strengthen health systems from the inside out. We don’t create parallel systems; we support ministries to integrate priorities into the policies and budgets they already own. This alignment is now more urgent than ever.
We support countries like Uganda and Ethiopia in developing Health National Adaptation Plans (HNAPs) through quantified climate risk assessments that move beyond analysis to action—building operational roadmaps with costed priorities, adaptation planning, and clear indicators. We work closely with governments to answer the question the GGA now makes urgent: What does a “resilient health service” look like in our context, and how will we know we’re getting there?
Persistent data and capacity gaps impede effective adaptation planning and the prioritization of the people and places most at risk, despite recent efforts by finance institutions. Only 44% of countries have costed their health adaptation needs, and existing finance falls short by billions. This mismatch between ambition and financing is now one of the greatest risks to implementation.
The Gap Between Ambition and Implementation
The new mental health indicator provides a perfect case study. Global recognition that climate change affects mental health is vital. But translating that into services requires ministries to train providers, adjust essential service packages, and create referral pathways that function even when roads are washed out. It requires community health workers who can recognize distress and provide first-line support. This is the granular, systems-strengthening work Pathfinder supports every day, turning a global metric into on-the-ground action. It also demonstrates that resilience is not only about infrastructure, but also about people and systems continuing to function under stress.

How We Measure What Matters
The demand for better finance tracking leads directly to a second imperative: proving impact. To attract and justify increased investment, we need robust, multi-level data that shows what works. This is where Pathfinder’s approach to monitoring offers a model.
We measure impact across the entire spectrum of health systems. Our programming uses indicators at the household level (reaching individuals and creating model households with composite metrics on health, finance, and emergency preparedness); the community level (strengthening health worker networks); the facility level (ensuring infrastructure, services, and supplies can withstand climate shocks); and the systems level (supporting national budgeting, vulnerability assessments, and planning).
For the last five years (2020–2024), our climate-resilience contributions include:
- More than 2,200 health facilities strengthened and became resilient to provide essential services during climate shocks.
- 14,500 health professionals trained to identify, prepare for, and respond to climate shocks.
- 25,000 youth climate advocacy leaders and champions trained.
- Reached 1 million community members to create “climate-friendly model households.”
- Built the climate resilience skills of 350,700 community members through climate and health awareness events.
These figures matter because they demonstrate that adaptation is measurable, and that investments can produce visible, trackable results. This multi-layered approach is exactly the kind of robust monitoring the finance community demands. It’s not just about counting outputs; it’s about demonstrating outcomes. By showing how a trained health workforce or a resilient facility maintains essential services during a climate shock, we provide the evidence base needed to make the case for smarter, more targeted adaptation finance.
The Missing Link: Tracking Climate-Health Finance
We have the indicators. We know how to implement them. But the entire system is undermined by a lack of transparent, needs-based financing. At COP30, after two weeks of negotiations, countries agreed to at least triple adaptation finance to $120 billion per year by 2035. While an increase on paper, this builds on a missed target from COP26 to double adaptation finance by 2025. The gap between rhetoric and reality remains vast.
Global public adaptation finance flows were only about $26 billion in 2023, highlighting how far the world still has to go. A recent report by The Rockefeller Foundation and SEEK Development highlights a core problem: current climate finance reporting is based on self-reported data with no verification or standardization. We simply cannot track financial flows against actual health needs with any accuracy. The report confirms that only 0.5% of multilateral climate funding supports health initiatives, forcing low-income countries to take on debt just to protect their populations’ health.
We can’t manage what we don’t measure. Building on the COP28 Guiding Principles, we need a consistent nomenclature for reporting climate-health financing. Public, transparent reporting on investment volumes, grant vs. loan ratios, and geographic distribution is not a bureaucratic exercise; it is the only way to ensure that commitments represent new financing, not just the reclassification of existing projects. Without this transparency, adaptation indicators risk becoming aspirational rather than transformational.
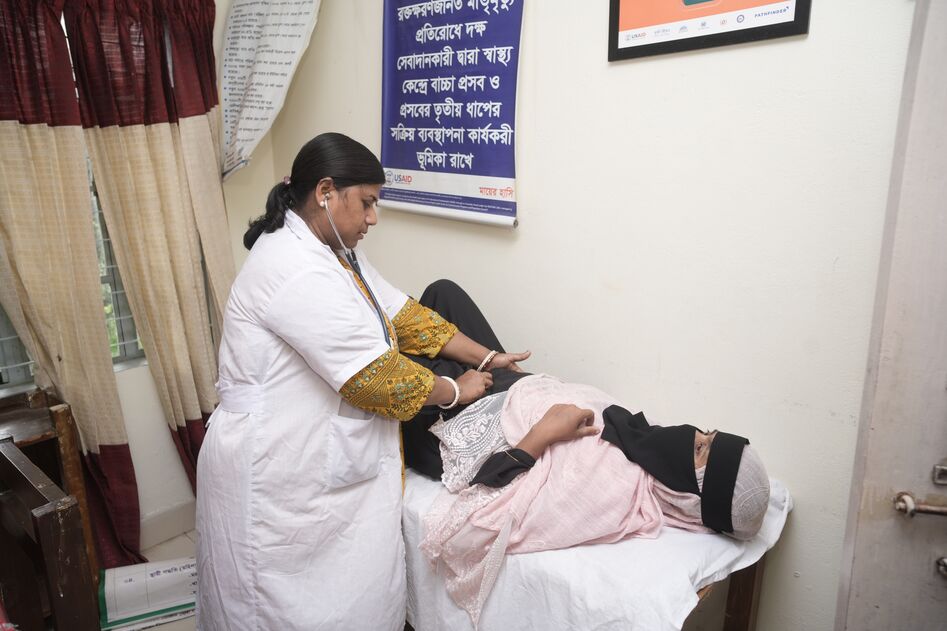
The Path Forward
The Lancet’s honest accounting of the procedural concerns at COP30, the last-minute changes, and the truncated negotiations are not minor footnotes. They reflect legitimate anxieties among the most climate-vulnerable countries that global frameworks can become unfunded mandates, or worse, tools for conditionalities.
When ministries own the process of selecting and adapting indicators, when they have the technical support to cost their adaptation priorities, and when they can demonstrate results to financiers, the framework becomes a tool for empowerment, not imposition.
Real accountability is ultimately domestic. It’s citizens holding their governments responsible for protecting health in a changing climate. It’s ministers of health making the case to ministers of finance that adaptation investments today prevent catastrophic costs tomorrow.
The COP30 framework gives the world a common language for adaptation progress. Pathfinder remains committed to helping governments speak that language fluently, not as a compliance exercise, but to ensure the resilient, equitable health systems every community deserves.
The indicators are adopted. The finance target is set. Now the test is whether the world can turn measurement into protection, and promises into lives saved.