Dr. Mengistu Asnake Kibret is Pathfinder’s Senior Country Director in Ethiopia. A public health physician with more than 30 years of experience in clinical service, program management, training, and operations research, he brings deep familiarity with Ethiopia’s public health system and its efforts to achieve Universal Health Coverage (UHC). Today, on International Health Coverage Day, Dr. Mengistu spoke with us about what it will take to achieve UHC and what achieving UHC would mean for Ethiopia.

Pathfinder advocates at the global level for UHC to be inclusive of sexual and reproductive health care. Why is sexual and reproductive health care an essential part of achieving UHC and what can countries do to ensure it is included?
UHC and sexual and reproductive health and rights (SRHR) are intimately linked. Without considering a population’s SRHR needs, UHC is impossible to achieve. Many basic health needs are linked to people’s SRHR—we see this every day through Pathfinder’s programs in Ethiopia. Similarly, universal access to SRHR cannot be achieved without countries defining a pathway toward UHC and prioritizing resources according to health needs.
To effectively meet the SRHR needs of all people, a comprehensive approach is required—one that provides an essential package of SRHR over the entire lifetime, and ensures equity in access to services and quality of care, without discrimination.
A comprehensive approach to SRHR is affordable for most countries, however, certain countries will need to make increased investments to achieve it. These countries must mobilize stakeholders, identify specific SRHR needs, map both resources available and systems constraints, and progressively implement interventions at various levels of the health system.

United Nations member states, including Ethiopia, recently renewed their commitment to achieving UHC. What should Ethiopia’s top three priorities be in order to reach this monumental achievement and why?
To achieve UHC, creating widespread access to comprehensive, high-quality health services and financial risk protection are essential. I believe that the strategies Ethiopia has developed through its renewed commitment to achieving UHC are practical steps that will enable the country to move rapidly toward UHC. Those strategies are:
- Defining Ethiopia’s Essential Health Service Package and identifying prioritized health interventions;
- Cost exemption or cost-sharing of high-priority interventions and expansion of community-based health insurance programs;
- Integrating health services within other sectors from the national to the district level to address social determinants of health and establishing emergency preparedness and response units at the national and regional level.
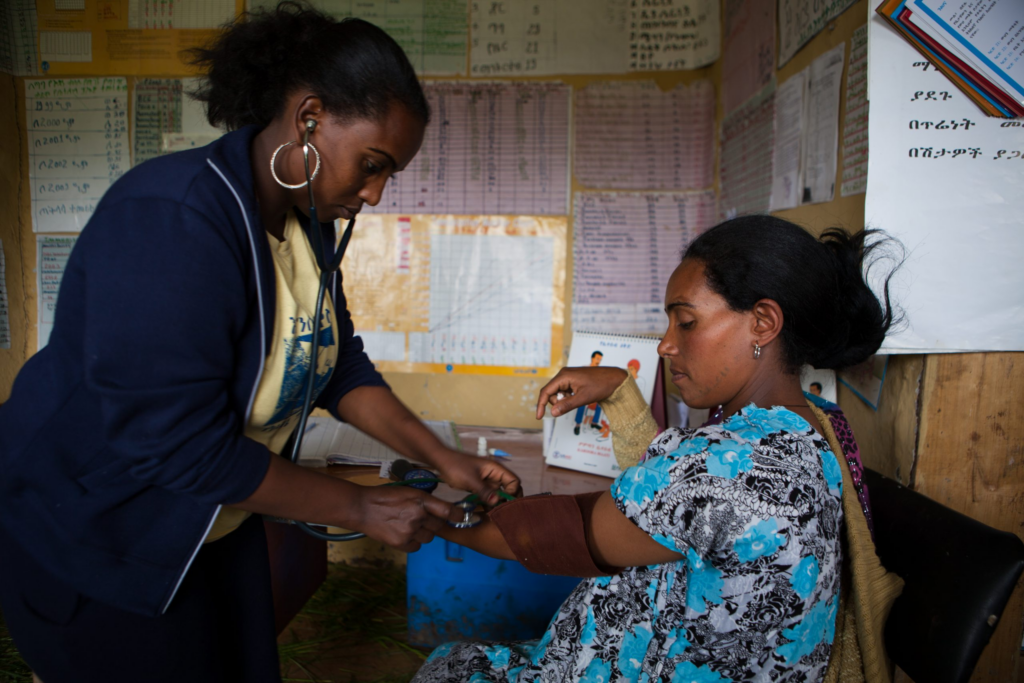
Given your in-depth knowledge of the public health system in Ethiopia, how has Ethiopia strengthened its primary health care (PHC) system over the past decade to meet the needs of women and girls and what must it further strengthen to meet the needs of all women and girls through UHC?
Ethiopia has been striving to achieve universal access to primary health care (PHC) since 2005. At the center of this effort has been the growth and development of the Health Extension Program. This program, staffed by close to 40,000 female Health Extension Workers (HEWs), has drastically improved access to quality community-based care, including sexual and reproductive health care, and health outcomes across the country. This important endeavor is backed up by professionals from district health centers who provide more comprehensive and quality health services to rural communities.
The success of PHC in Ethiopia, however, depends not just on policy statements, resource reallocations, and expansion of health infrastructure, but also on a fundamental change in attitudes and values regarding the development of human resources and the equitable distribution of social services. Going forward, the government must improve health care insurance, motivate and incentivize HEWs to provide quality services, equitably distribute health professionals, ensure availability of supplies and commodities across regions, and build strong linkages with community members and networks.
Ethiopia is a pioneer in piloting and scaling up community-based health insurance as a means of achieving UHC. Why did Ethiopia choose this approach and what learning does Ethiopia have to share with other African countries considering the same?
The World Health Organization’s definition of UHC is a situation where all people who need health services receive them, without incurring financial hardship. This entails two interrelated components: coverage with needed quality health services and access to financial risk protection, for everyone.When people must pay most of the cost for health services out of their own pockets, the poor are often unable to obtain many of the services they need, and even the rich may be exposed to financial hardship in the event of severe or long-term illness. Pooling funds from compulsory funding sources (such as mandatory insurance contributions) can spread the financial risks of illness across a population.
The Government of Ethiopia introduced community-based health insurance and social health insurance in 2011 to address these hardships. The program has grown over time, increasing membership enrollment and renewal rates, increasing the mobilization of domestic resources, and improving use of health services. It has empowered community members, particularly women and girls, to be very assertive in demanding their right to health and well-being, and creating social accountability.

What would achieving UHC mean for Ethiopia, in terms of health and well-being, economic growth, women’s empowerment and gender equality, and development generally?
UHC would go a long way in achieving women’s empowerment and gender equality, and that’s why Pathfinder stands behind the charge for UHC internationally. In most developing countries, the household economy is managed by men, and women who seek health care will not go to health facilities for health services as they have little or no control over money. Through UHC, such problems will be resolved. Most maternal and child health services are made free of charge and other health services will become accessible to women, girls, and children through community-based health insurance.
Since UHC enables everyone access to services that address the most significant causes of disease and death and ensures that the quality of those services is sufficient to improve the health of the people who receive them, the productivity of the young generation will drastically improve. The low spending on health due to quality of services, low out-of-pocket expenditures, use of additional resources for other development issues, and so on would have a snowballing effect to the overall development of the nation.












