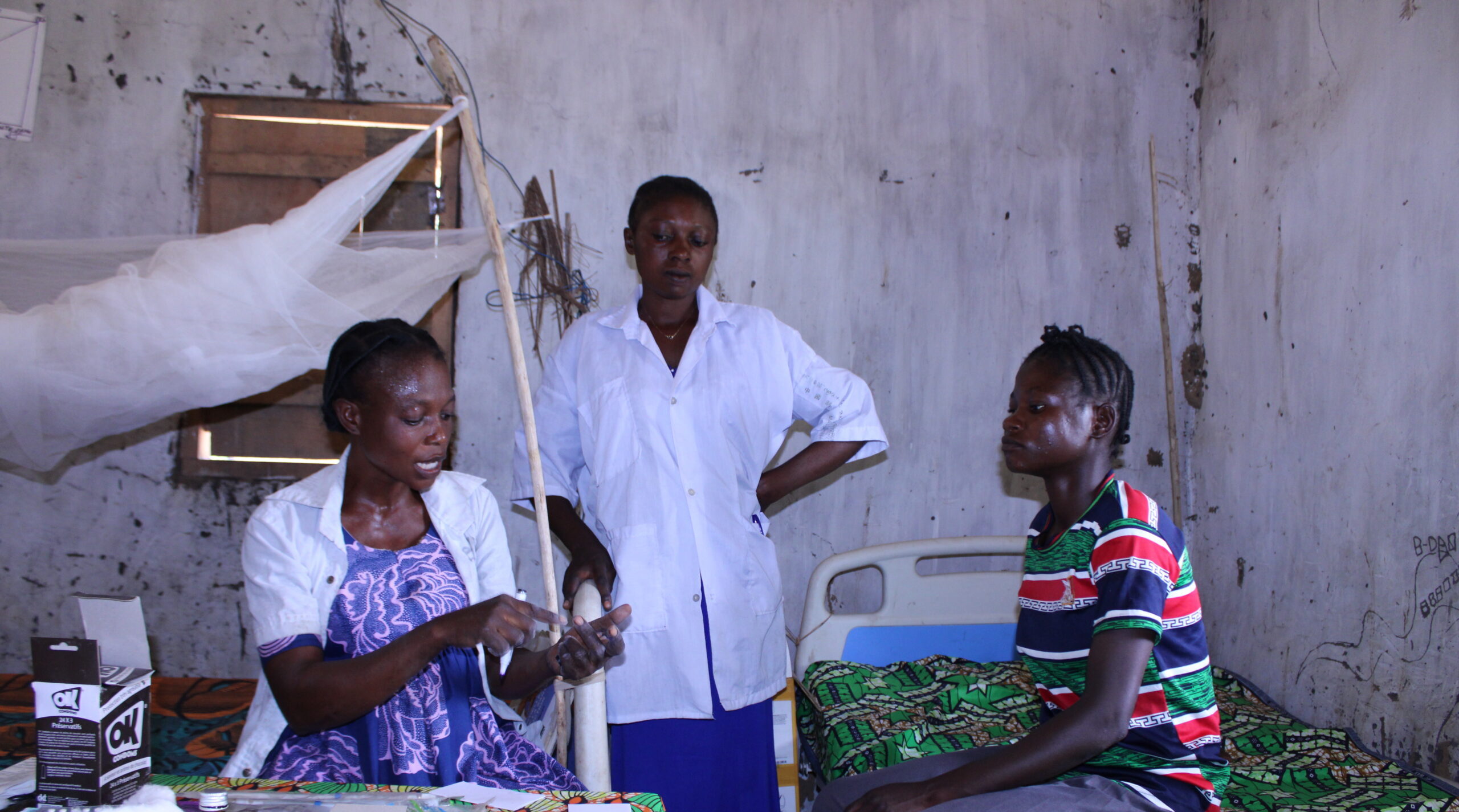I Used to Fear it. Now I Master it.
KIKWIT, Democratic Republic of the Congo — For years, women in Kwilu Province faced a frustrating reality: they would walk into a health clinic seeking family planning services and leave empty-handed. Not because contraceptives were unavailable on the shelves, but because health care providers lacked the confidence and skills to offer them.
IUDs and implants sat unused in storage while women were quietly steered toward methods requiring less technical expertise. The reason was not patient preference—it was provider anxiety.
“Before the PMNS-PF project (Projet Multisectoriel de Nutrition et de la Santé, or Multisectoral Nutrition and Health Project), I had never been trained in family planning,” said a nurse from Plateau I Health Center in Kikwit North. “Inserting an IUD—including hormonal IUDs—or placing and removing an implant gave me anxiety.”
This scenario was all too common across Kwilu Province. The DRC’s National Strategic Plan for Family Planning (2021–2025) identified this gap clearly: health care providers needed practical, hands-on training—not just classroom theory, but real mentorship at the point of care.
“Before the PMNS-PF project, I had never been trained in family planning. Inserting an IUD or implant was a source of anxiety for me. With training and clinical mentorship—observation, supervised practice, debriefing—everything changed. Today, I have mastered these procedures and I better support clients in making informed choices because they deserve better.”
—Nurse, Plateau I Health Center, Kikwit North Health Zone
A Turning Point: Mentorship at the Bedside
Enter clinical mentorship, an approach that brings expert guidance directly to health care facilities. Through the PMNS-PF project, implemented by SANRU and Pathfinder International with World Bank funding, 96 mentors were trained across 24 health zones in Kwilu Province.
Unlike traditional training that ends when participants leave the classroom, clinical mentorship is ongoing and intimate. Mentors observe providers during actual patient consultations, offer real-time guidance, supervise practice, and debrief afterward. It is learning that happens where it matters most: at the bedside.
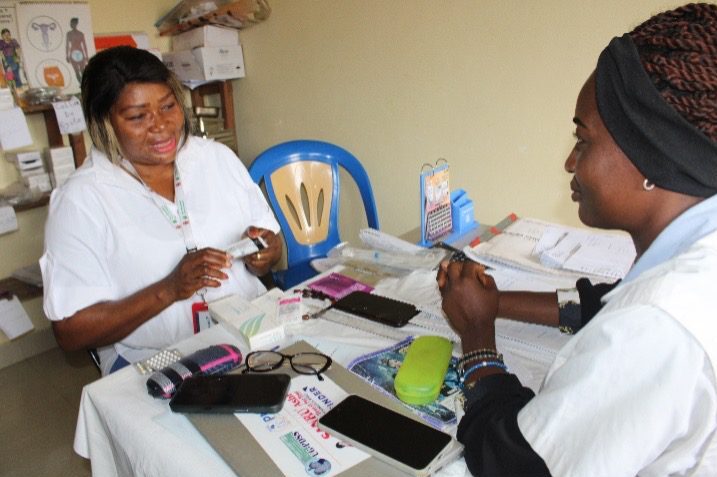

At the Misay 1 Hospital Center in the Kikongo Health Zone, Irène Bule embodies this transformation. When her more experienced colleague was transferred to another facility, Irène was suddenly thrust into the role of family planning provider—with minimal training.
“I like offering family planning services, but before, it was a more experienced colleague who handled it,” Irène recalls. “After her transfer, the head nurse designated me as a mentee.”
Her mentor, Blaise Munkanga, a supervising nurse in Kikongo Health Zone, began regular visits. “With him,” says Irène, I went from almost zero to a competent provider. Today, I have mastered all the techniques. What I love most is following the technical checklist step by step. The more I use it, the more I have memorized it—my mastery strengthens with every review.”
Blaise mentors providers across three health facilities and has witnessed countless similar transformations. “We often face staff instability—trained providers move or get transferred, leaving a gap in facilities. Now we mentor at least two providers per facility to ensure continuity even when someone leaves.”
“In just three months of regular mentorship sessions, a provider reaches an impressive level of mastery. I have noticed that young women providers progress very quickly in rural areas.”

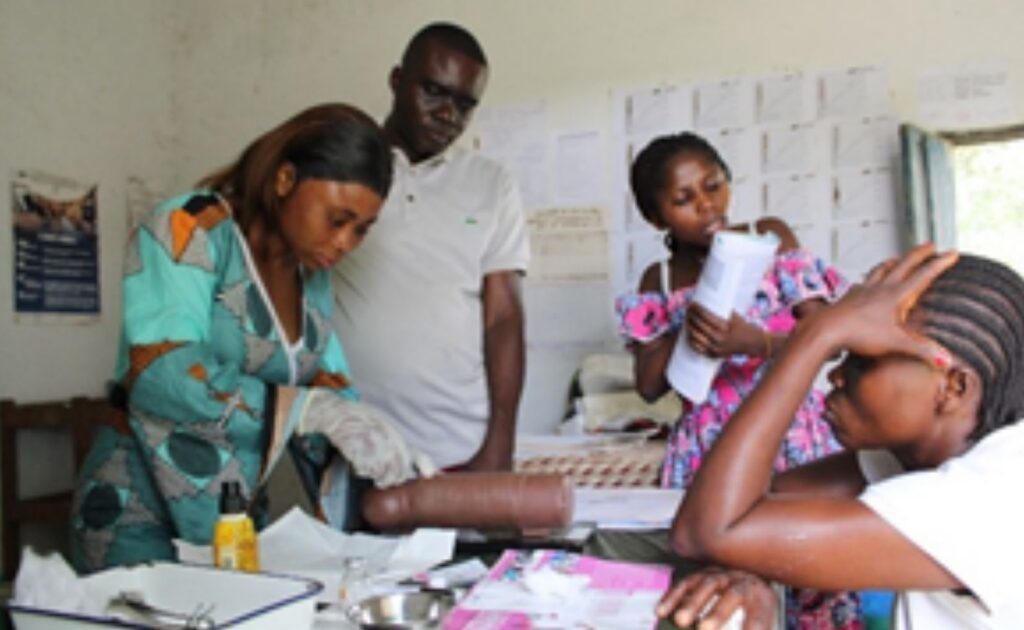
A Ripple Effect
The impact extends far beyond individual health care workers. Nedine Ndeke, head of family planning services and a mentee in Mukula Nzadi, sees the broader picture: “In our health area, women finally have access—close to home—to family planning that is safe, respectful, and truly available.”
Each of the 240 mentored providers supervises five community-based distributors in their health areas, exponentially expanding the reach of quality family planning services.
Building a Sustainable System
The 96 trained mentors are supported by Project Advisors who conduct monthly field visits alongside Central Office staff from Health Zones. Each advisor follows eight mentors—four per health zone—ensuring quality standards across the province.
The mentorship relationship is defined as a reciprocal learning partnership: mentor and mentee work together toward mutually defined goals that develop the mentee’s skills, capacities, knowledge, and critical thinking.
At the head of the program sits Dr. Patrick Kabeya, Senior Technical Advisor for Reproductive Health and Family Planning. Dr Kabeya provides strategic oversight for the program across both Kwilu and Kasai provinces—from priority-setting to quantifying contraceptive commodities to ensure consistent availability.
“What I appreciate most,” says nurse Venance Gihalu Sembu, is being able to offer quality services, free of charge thanks to the project, and seeing the satisfaction of the women we serve. For us providers, it is motivating to feel our skills improving with each mentor visit.”

Looking Ahead
The success in Kwilu Province offers a roadmap for scaling quality family planning services across the DRC and beyond. By investing in health care providers through sustained, practical mentorship, the PMNS-PF project proves that technical skills—and confidence—can be built over time.
For the 1,107,477 women who received modern family planning services in 2025, that gift translates into something profound: the power to make informed choices about their own bodies, their families, and their futures.
“Our project turns policy into concrete change at health facilities in Kwilu,” says Dr. Jackson Kipulu, Reproductive Health & Family Planning Specialist. “Clinical mentorship visits at the workplace—observation, supervised practice, debriefing—national quality assurance guidelines to standardize every procedure and counseling step, and logistical support to reduce supply disruptions.”
Results in 2025
- 96 mentors providing clinical mentorship
- 24 health zones covered in Kwilu Provincial Health Division
- 720 mentorship visits conducted
- 681 mentees trained. This includes 240 providers who were previously trained in family planning and 441 providers who were not previously trained.
- 1,107,477 women using modern family planning methods.
- 99,763 women who received postpartum modern family planning services.