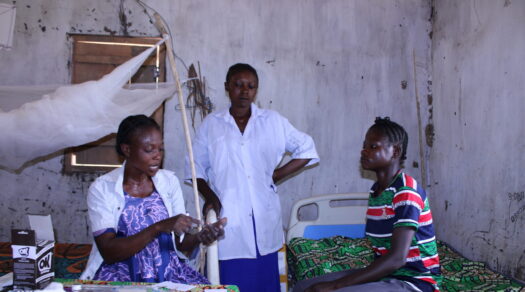Cervical cancer is a tragedy—a completely avoidable one.
We have the knowledge, tools, and technologies to eliminate cervical cancer, yet the disease remains a leading cause of cancer deaths for women in too many countries.
In most regions of the world, more women now die from cervical cancer than from pregnancy-related complications. In 2018, there were 569,847 new cases of cervical cancer and 311,365 women died from the disease.
Low- and middle-income countries account for 90% of the cervical cancer cases. In my country alone, 4,884 Ethiopian women died of cervical cancer just last year.
In high-resource settings, the invention of the “Pap smear” and subsequent screening and treatment have drastically reduced the number of cervical cancer deaths. In low- and middle-income countries, however, women often lack necessary information and don’t have access to prevention and treatment services.
Cervical cancer screening and preventive treatment are a “best buy” in public health. The screening and preventative action reduce the cost of treating pre-cancer and invasive cervical cancer and prevent women’s lost productivity at the peak of their working lives.
Cervical cancer screening and treatment is endorsed by the World Health Organization’s Global Call to Action as a best buy. Yet only 22 countries currently achieve screening rates of 70% or more.
Addis Tesfa
Ethiopia takes the cervical cancer crisis seriously.
Pathfinder, with Ethiopia’s Ministry of Health and Stanford University’s Program for International Reproductive Education and Services and support from the US Centers for Disease Control and Prevention, introduced the first pilot cervical cancer prevention and control project in 2009 called Addis Tesfa. This five-year project initially targeted HIV+ women who are at the greatest risk for developing cervical cancer because their immune systems are unable to fight off human papillomavirus (HPV), which causes cervical cancer.
Addis Tesfa adopted the WHO’s “single-visit approach,” or SVA. SVA combines visual inspection of the cervix with an acetic acid wash (vinegar) that highlights abnormal cells, and same-day treatment of pre-cancerous lesions with cryotherapy or referral of women with advanced lesions for Loop Electrosurgical Excision Procedure (LEEP).
Community education and engagement, combined with training health facility staff, enabled 33,000 eligible women to receive cervical cancer screening at 32 public hospitals.
In total, 2,883 women—93% of those who screened positive for precancerous lesions—were treated with cryotherapy or LEEP.

I would like to remind all my sister women that they should waste no time to save their life from the threat of cervical cancer since the screening and treatment is too simple, said Yewube Ayalew, pictured above. Yewube was treated for cervical precancerous lesions through Addis Tesfa.
A national prevention and control program
Building on the experience of Addis Tesfa, the Ethiopian Ministry of Health has been scaling up cervical cancer prevention and control nationally since 2015. The program currently operates in 220 public health facilities, with plans to expand to 800 facilities, or one health facility per district.
The national program follows key policies and guidelines adopted by the Ministry of Health that integrate SVA into the national reproductive health strategy. Cervical cancer prevention through SVA is now considered an essential part of a comprehensive women’s health package that includes sexual and reproductive health care—as it should be.
While the national prevention and control program is saving the current generation of women through early detection and treatment, the Ministry of Health launched a vaccination campaign in December 2018 to save the next generation. The Ministry of Health has pledged to vaccinate 1 million 14-year-old girls against HPV.
Beyond Ethiopia’s borders
Using the lessons learned in Ethiopia, Pathfinder began expanding its cervical cancer prevention work in 2016 to Burundi, Mozambique, Nigeria, and Tanzania, aiming to create a cervical cancer prevention network in sub-Saharan Africa. Ethiopia has served as the training and knowledge transfer hub for high-impact and promising practices. Close to 10,000 women have received screening at 13 health facilities in the four countries, and more than 500 women have been treated for precancerous lesions.
Each country has adapted the lessons learned from Ethiopia to their own contexts and to align with ongoing programs. In Mozambique, for example, the program is reaching sex workers who are at great risk of cervical cancer. In Tanzania, task-sharing has engaged community health workers in the program to meet human resource gaps. These adapted programs can provide rich learning for cervical cancer prevention in other low- and middle-income countries.
Partnership is the way forward
To continue to advance cervical cancer prevention globally, Pathfinder has joined the TogetHER partnership—engaging in advocacy and supporting programs positioned to eradicate cervical cancer.
We also continue to partner with the national program in Ethiopia—we recently collaborated with the Ministry of Health to introduce use of the Enhanced Visual Assessment Device at four university hospitals. The new technology will improve visual inspection of the cervix, making it easier to identify treatable precancerous lesions and ultimately saving more lives.